The peptidic post-translational modifiers of the Ubiquitin Family (UbL) are reversibly conjugated to thousands of cellular proteins, the activity, function and/or fate of which they modify. In this way, they play a role as important as that of phosphorylation in virtually all cellular processes. In particular, they are essential for the control of gene expression and is disrupted in a variety of disease situations.
In this context, we are studying how UbL, in particular SUMO, notably through their ability to regulate gene expression programs, are involved in the response of Acute Myeloid Leukemia (AML) to therapies, as AML is a hematological malignancy with a poor prognosis whose treatment has not changed significantly in 40 years.
We have shown that SUMOylation controls AML cells response to chemotherapeutic drugs (anthracyclines such as daunorubicin or idarubicin and nucleoside analogues such as aracytin) used in standard AML treatments (Bossis et al., Cell Reports, 2014; Boulanger et al., Nucleic Acids Research, 2023) as well as to differentiation therapies using All-trans-retinoic acid (Baik et al., Cancer Research 2018). In addition, we have shown that deregulation of SUMOylation and ubiquitylation enzyme activity is associated with AML resistance to standard chemotherapies (Gâtel et al., Life Science Alliance, 2020) and might serve as a biomarker of AML response to these treatments (patent EP19305688, 2019).
SUMOylation inhibitor TAK-981 synergizes with Azacitidine in preclinical models of Acute Myeloid Leukemias and limits immune escape
The recent discovery of TAK-981 (Subasumstat), a first-in-class SUMOylation inhibitor, has allowed us to test in preclinical models the therapeutic relevance of targeting the SUMO pathway in AML. We could show that TAK-981 is endowed with potent anti-leukemic activity in various preclinical models of AML. TAK-981 targets AML cell lines and patient blast cells in vitro and in vivo in xenografted mice with minimal toxicity on normal cells. Moreover, it synergizes with 5-azacitidine (AZA), a DNA-hypomethylating agent now used in combination with the BCL-2 inhibitor venetoclax to treat patients unfit for standard chemotherapies. Interestingly, TAK-981+AZA combination shows higher anti-leukemic activity than AZA+venetoclax combination in vivo, at least in the model tested. Mechanistically, TAK-981 potentiates the transcriptional reprogramming induced by AZA, promoting differentiation and death of the leukemic cells. In addition, TAK-981+AZA treatment induces many genes linked to inflammation and immune response pathways. In particular, it leads to the secretion of type I interferon (IFN-I) by AML cells. Finally, TAK-981+AZA induces the expression of Natural Killer (NK)-activating ligands (MICA/B) and adhesion proteins (ICAM-1) at the surface of AML cells. Consistently, TAK-981+AZA-treated AML cells activate NKs and increase their cytotoxic activity. Targeting SUMOylation with TAK-981 may thus be a promising strategy to both sensitize AML cells to AZA and reduce their immune-escape capacities (Gabellier et al, Haematologica, 2023).

SUMOylation represses the anti-leukemic innate immune response by controlling the interferon pathway
In addition to its effects on cancer cells, recent studies suggest that targeting SUMOylation activates both the innate and adaptive antitumor immune responses. Given their critical role in antitumor surveillance in AML, we focused on natural killer (NK) cells. We showed that inhibition of SUMOylation activates NK cells from healthy donors and patients, enhances their cytotoxicity toward AML cells, and increases their cytokine secretion capacity(IFN-γ, TNF-α, FasL). In vivo, TAK-981 improves the anti-leukemic efficacy of ex-vivo expanded cord-blood NK cells in leukemia-bearing mice. One early effect of TAK-981 is to specifically increase the accessibility and activation of cis-regulatory regions of type I interferon (IFN-I) pathway genes and induce their transcription. TAK-981-induced secretion of interferon-β, mostly by NK cells and myeloid cells, is required for NK cells activation. Surprisingly, IFNB1 induction does not require its best-characterized activators MDA5, cGas, IRF-1, -3 and -7. Altogether, this suggests that targeting SUMOylation activates a non-canonical IFN-I pathway, which enhances the anti-leukemic potential of NK cells. (Hallal et al., Molecular Cancer Therapeutics, 2025).
Hence, inhibition of SUMOylation could (i) restore NK cell activity in patients and (ii) enhance the anti-leukemic efficacy of donor-derived NK cells, with potential applications in the context of allogeneic transplantation.
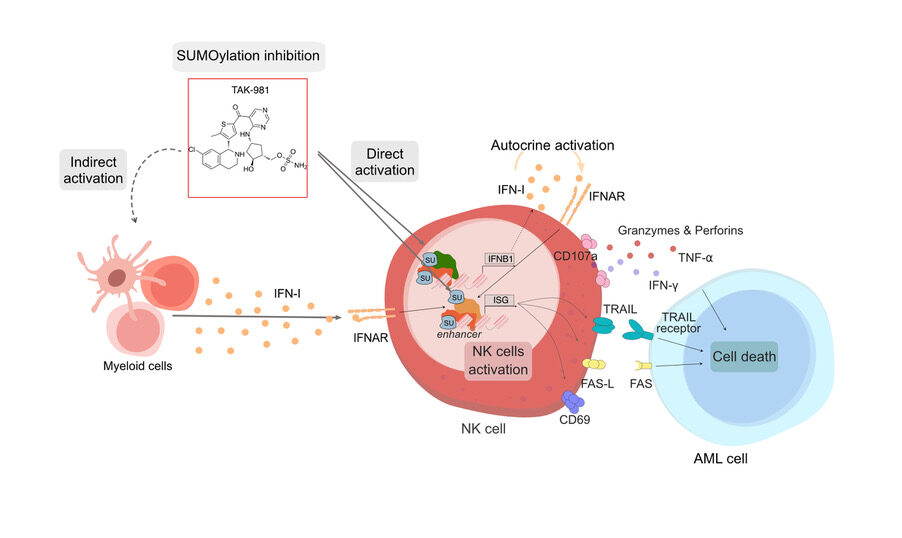
Our current work at better understanding, at the molecular level, the role of SUMOylation in (ii) the response of AMLs to therapies (chemotherapies, differentiation therapies and epidrug-based therapies), (ii) the activation of an anti-tumor immune response. We also aim to further validate, in preclinical models of AMLs, the efficacy of SUMOylation targeting in the treatment of AMLs, alone or in combination with existing therapies. This work is carried out in close collaboration with the Department of Clinical Hematology of the University Hospital of Montpellier. Finally, we are developing new tools and molecules to target SUMOylation in AML and more generally cancer, in particular through our ongoing collaboration with Dr Muriel Amblard’s team (IBMM).